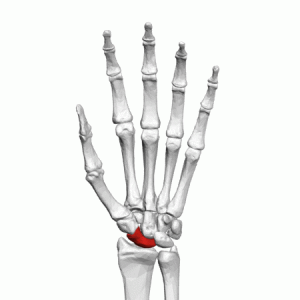
 The scaphoid, or navicular, is the most commonly fractured carpal bone in the wrist. The scaphoid is almost completely covered in articular cartilage and functions like a ball bearing in the wrist joint. Its blood supply is very fragile and a fracture often leaves the bone without any blood flow, which makes healing this bone very difficult. Because of this, Dr. Viola is very aggressive in treating acute scaphoid fractures in order to see them heal primarily. Often times, however, patients break their scaphoid and do not know it. Delayed treatment (months, years) can lead to avascular necrosis (loss of blood supply), non-union, loss of wrist motion and function and painful arthritis. When this happens, treatment of the chronic non-union scaphoid is necessary.
The scaphoid, or navicular, is the most commonly fractured carpal bone in the wrist. The scaphoid is almost completely covered in articular cartilage and functions like a ball bearing in the wrist joint. Its blood supply is very fragile and a fracture often leaves the bone without any blood flow, which makes healing this bone very difficult. Because of this, Dr. Viola is very aggressive in treating acute scaphoid fractures in order to see them heal primarily. Often times, however, patients break their scaphoid and do not know it. Delayed treatment (months, years) can lead to avascular necrosis (loss of blood supply), non-union, loss of wrist motion and function and painful arthritis. When this happens, treatment of the chronic non-union scaphoid is necessary.
Causes
Scaphoid fractures are the result of a traumatic fall on an outstretched and hyperextended hand (FOOSH). Although the bone is small, it takes a large force to break it. Men are 10x more likely to break this bone than women.
Signs and Symptoms
Pain is typically felt on the radial (thumb-side) aspect of the wrist and may only last a few days. There is some degree of swelling and there may be somewhat limited wrist mobility. Bruising is rare and there is often no visible deformity of the wrist, which makes people think they have just “sprained” their wrist. This can delay the treatment of the fracture, which can make it difficult to treat down the road.
Diagnosis
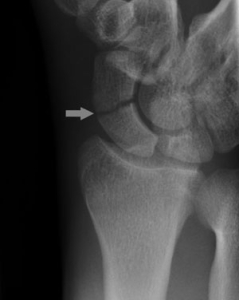 Diagnosing a scaphoid fracture can be difficult because the fracture is not always obvious on plain film x-rays, especially if the fracture is non-displaced. With an appropriate history, physical exam findings of tenderness in the region of the scaphoid (the “anatomic snuffbox”) there should be high clinical suspicion for a fracture and it should be treated as such until proven otherwise. The consequences of under treating a scaphoid fracture can lead to non-union and wrist arthritis. In all questionable cases, Dr. Viola recommends an MRI or CT scan to help with the appropriate diagnosis and immediate treatment.
Diagnosing a scaphoid fracture can be difficult because the fracture is not always obvious on plain film x-rays, especially if the fracture is non-displaced. With an appropriate history, physical exam findings of tenderness in the region of the scaphoid (the “anatomic snuffbox”) there should be high clinical suspicion for a fracture and it should be treated as such until proven otherwise. The consequences of under treating a scaphoid fracture can lead to non-union and wrist arthritis. In all questionable cases, Dr. Viola recommends an MRI or CT scan to help with the appropriate diagnosis and immediate treatment.
Treatment
If the fracture is non-displaced, most hand surgeons may treat this injury in a long-arm and then eventually short-arm cast for a total 6-12 weeks (or more) and there is still a chance that the blood supply is disrupted and that healing may not take place despite complete immobilization for that period of time. Often, in order to prevent prolonged casting of a non-displaced fracture and to help ensure that it heals primarily, Dr. Viola’s recommendation is to surgically place a screw in the broken scaphoid. This reduces the fracture and realigns the bone so that the broken pieces are held together and the fragile blood supply can help heal the bone. Sometimes, however, the fracture is displaced and in a region where the blood supply is known to be especially poor and surgical fixation is the necessary to prevent nonunion and avascular necrosis.
Surgical Fixation
Because the scaphoid fracture is such a common injury, Dr. Viola has devised a device to help make surgical fixation even easier on the surgeon and the patient’s recovery. A larger guide wire is drilled through the patients skin to reduce the fracture and drill the hole for the compression screw and another wire is used to measure for the appropriate screw length. Then, a very tiny incision is made in the skin in order to insert the cannulated PET Device (percutaneous exchange tube) over the wire, which is then anchored into the distal end of the scaphoid. This allows for easy exchange (while maintaining reduction of the fracture) of the larger guide wire, which is replaced with a smaller one that the cannulated titanium compression screw fits over. The compression screw is then very carefully screwed into the bone by hand (not power). The surgeon needs to make sure the ends of the bone come together perfectly so that the blood supply is also properly restored. The PET device is removed and the skin is closed with a steri-strip or suture. If the patient is to be very active post-operatively, a short-arm cast or splint is applied in a couple of days for extra-protection for a few weeks.
Watch Full Surgery
Non-Union and Avascular Necrosis
If a scaphoid fracture is not recognized, undertreated or treatment is delayed, it will most likely not heal and go onto become a non-union. Sometimes, even with treatment in a cast the fracture may not heal due to poor blood supply and the bone dies (avascular necrosis). Collapse of a dead scaphoid bone can further lead to mal-alignment within the wrist and subsequent arthritis, which can be very painful. If this is found before arthritis has developed, reconstruction of the dead scaphoid may be performed. This reconstruction involves obtaining vascularized bone graft from the distal radius, which is a piece of bone that has an artery attached to it that gets “built in” to the new scaphoid so that a new blood supply is fed into the scaphoid. More bone graft is obtained from the hip or leg and packed around the other graft and secured with screw fixation in order to restore the shape and blood supply of the original scaphoid.
Post-traumatic Arthritis
If radial-carpal arthritis with severe wrist pain has developed because of severely delayed treatment, usually of several years, patients are often candidates for partial or total wrist fusions where there is removal of the degenerated scaphoid bone and partial or complete fusion of the wrist joint, depending on the severity of arthritis.
Learn How We Can Help You Stay Active

